Humans have three blood groups- A, B and O.
According to previous studies, it was said that Type A blood had higher risks of catching COVID-19 and Type O blood had the least risk.
Now according to a study conducted last week, the early findings and conclusions about the probability of a certain blood group being prone to catch the virus faster has been disproved. This study shows that there is no evidence of blood groups playing a role in catching the virus.
So what are blood groups for actually?
Even scientists are baffled over this question. Over a course of evolution, we have three different blood groups, but so far there isn’t any conclusive study that tells us as to what disease can be linked by what blood group or why we have different blood groups as well.
A brief 101 on blood groups-
Technically, like all genetic traits, you tend to inherit your blood group from your parents as well. And apart from transfusion processes – which is a lifesaving procedure, blood groups don’t really matter much.
The first person to initiate blood transfusions was the Pioneering physician Dr. James Blundell, who worked in London in the early 1800s, gave blood transfusions to 10 of his patients — only half survived. What he didn’t know is that humans should only get blood from certain other humans.
The reason? Your ABO blood group is identified by antibodies, part of the body’s natural defense system, and antigens, a combination of sugars and proteins that coat the surface of red blood cells. Antibodies recognize any foreign antigens and tell your immune system to destroy them. That’s why giving someone blood from the wrong group can be life-threatening.
For example, I have type A+ blood. If a doctor accidentally injected me with type B, my antibodies would reject and work to break down the foreign blood. My blood would clot as a result, disrupt my circulation and cause bleeding and difficulties breathing — and I would potentially die. But if I received type A or type O blood, I would be fine.
Your blood type is also determined by Rh status – an inherited protein found on the surface of red blood cells. If you have it, you’re positive. If you don’t, you’re negative.
Most people are Rh positive, and those people can get blood from negative or positive blood type matches. But people with Rh-negative blood typically should only get Rh-negative red blood cells (because your own antibodies may react with the incompatible donor blood cells.)
That leaves us with eight possible primary blood types, although there are a few more rare ones.
Here’s the transfusion chart that explains which blood groups can be donors and receivers for transfusion:
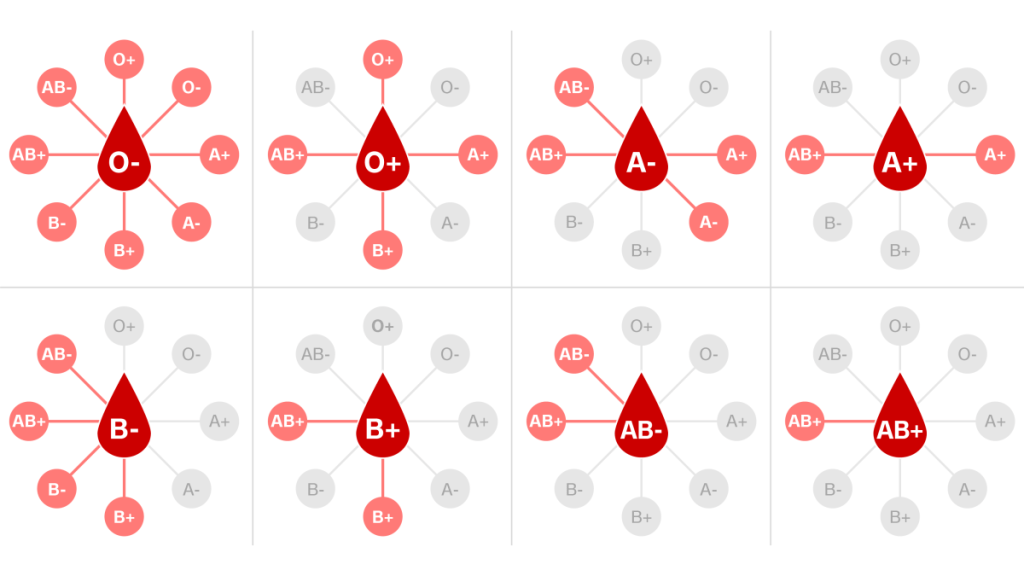
So what does that have to do with the Coronavirus?
A handful of studies have shown a link between blood type and the novel coronavirus, though most involved a small number of people and some were not peer reviewed.
A team of European researchers who published their findings in the New England Journal of Medicine in June found people with Type A blood had a 45% higher risk of becoming infected than people with other blood types, and people with Type O blood were just 65% as likely to become infected as people with other blood types. They studied more than 1,900 severely ill coronavirus patients in Spain and Italy, and compared them to 2,300 people who were not sick.
A similar effect for Hong Kong health care workers with blood group O was observed during the SARS outbreak, which infected 8,098 people from November 2002 to July 2003 and is from the same family of viruses.
Last week’s study may counter some of that research. “We showed through a multi-institutional study that there is no reason to believe being a certain ABO blood type will lead to increased disease severity, which we defined as requiring intubation or leading to death,” said Dr. Anahita Dua of Mass General, who led the study team.
There are two hypotheses about the link between blood groups and Covid-19, said Jacques Le Pendu, research director at Inserm, a French medical research organization. One is that people with type O are less prone to coagulation problems and clotting has been a major driver of the severity of Covid-19.
He said it could also be explained by the likelihood that the virus will carry the infected person’s blood group antigen. As such, the antibodies produced by a person with blood group O might neutralize the virus when caught from a person with blood group A — similar to the rules for blood transfusions.